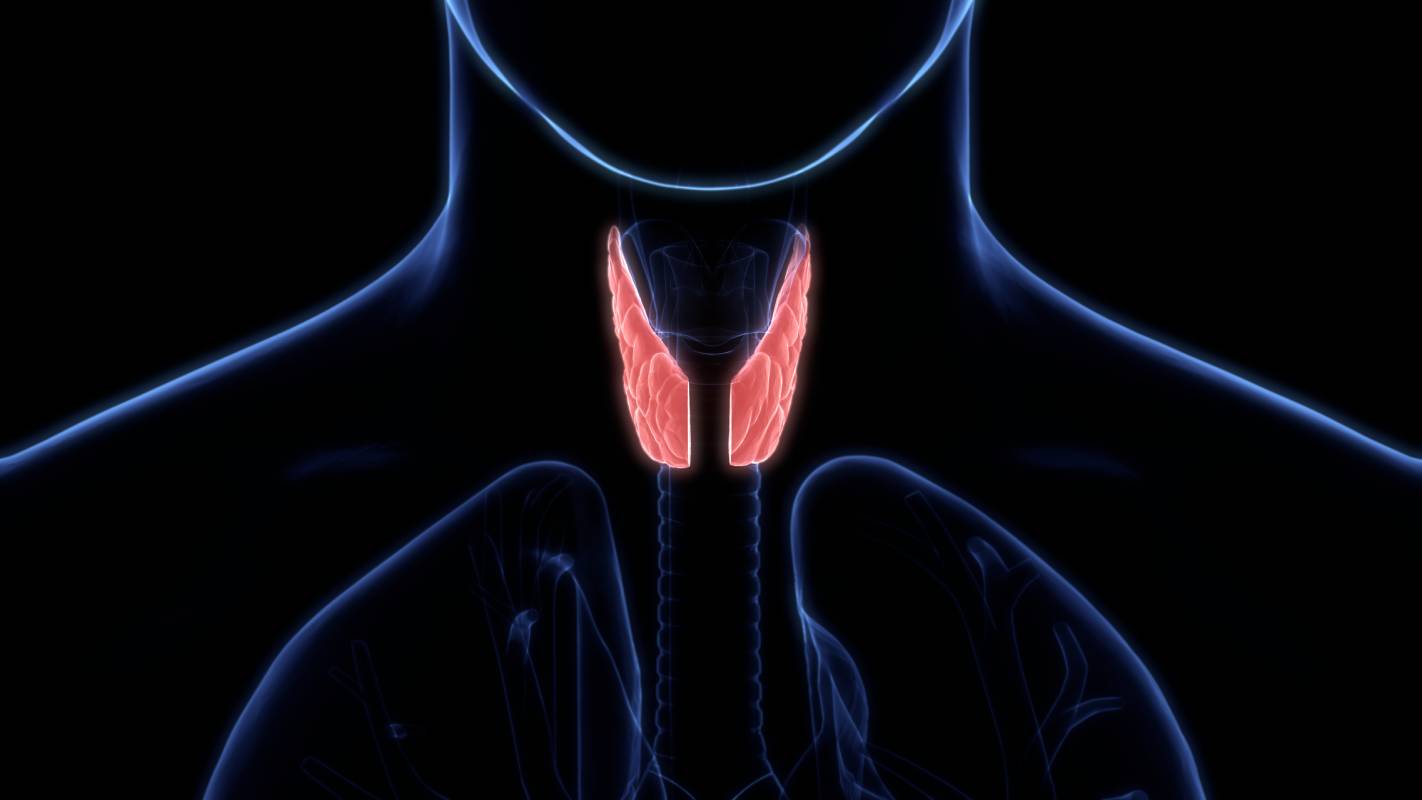
The thyroid is a gland located in the anterior region of the neck and is a critical part of the endocrine system.1 Specifically, the thyroid secretes the hormones T3 and T4, which increase the body’s basal metabolic rate, and calcitonin, which lowers blood calcium.2 Partial or complete removal of the thyroid in an operation known as a thyroidectomy may be recommended when cancer is detected or suspected to exist in the thyroid.3 Thyroid surgery may range from the simple removal of a small nodule from the thyroid to a more complicated operation to relieve the trachea from the pressure caused by a goiter (swelling of the neck resulting from enlargement of the thyroid), and the optimal anesthesia approach is affected by the type of surgery as well as patient factors.
Several different anesthesia options exist for thyroid surgery. Regional anesthesia has been shown to be effective and safe, though it is more often used for procedures on smaller scales.4 More common for a thyroidectomy, however, is general anesthesia. When tracheal compression is occurring, anesthesia can usually be administered without any impediments, however, a patient may be induced into the semi-supine or sitting position or, in more extreme cases, undergo fiberoptic intubation if needed.5 Pre-oxygenation with 100% oxygen should precede muscle relaxation for general anesthesia.
Total intravenous anesthesia, which is the use of intravenous agents only for the induction and maintenance of anesthesia, is commonly used during thyroid surgery.6 Propofol is among the most effective anesthetic agents, as it provides a rapid onset of anesthesia, does not have an extended recovery time, and has a low incidence of postoperative nausea.7 Opioids are often co-administered to potentiate their effect: the combination of propofol with the opioid remifentanil provides a short duration of action that can be easily targeted as well as adjusted for specific patient needs.8
There are several potential postoperative complications that anesthesiologists must be careful to detect and prevent from developing. One such complication is recurrent laryngeal nerve (RLN) palsy, a condition in which the recurrent laryngeal nerves that control the muscles of the larynx become injured, which can result in hoarseness, difficulty breathing, and physical exhaustion.9 While permanent nerve palsy occurs in less than 2% of patients undergoing thyroid surgery, temporary palsy has been reported in 3-10% of patients.10 The condition can be brought about by contusion to or clamping of the nerves during intubation and extubation, and, as such, anesthesiologists traditionally inspect the vocal cords immediately after extubation.5 Since this is often technically difficult, anesthesiologists can use a fiberscope or electrophysiological monitoring to prevent damage to the RLNs.11 An additional potential postoperative complication is postoperative hemorrhage, which can be avoided by maintaining hemostasis. Anesthesiologists typically maintain the patient’s intrathoracic pressure for 10-20 seconds to ensure that hemostasis has been achieved before the wound is closed.7
The parathyroid is a gland adjacent to the thyroid that maintains calcium homeostasis, and a parathyroidectomy, like a thyroidectomy, is a common surgical procedure for parathyroid swelling. In contrast to the thyroidectomy, however, local anesthesia is typically used for a parathyroidectomy, which may involve cervical nerve blocks.5 Nerve blocks may be deep or superficial, though no significant differences in postoperative pain and patient satisfaction have been found between the two types.
References
1. Beynon, M. E. & Pinneri, K. An Overview of the Thyroid Gland and Thyroid-Related Deaths for the Forensic Pathologist. Acad. Forensic Pathol. 6, 217–236 (2016).
2. How does the thyroid gland work? InformedHealth.org [Internet] (Institute for Quality and Efficiency in Health Care (IQWiG), 2018).
3. Thyroid Surgery. American Thyroid Association https://www.thyroid.org/thyroid-surgery/.
4. Hisham, A. N. & Aina, E. N. A reappraisal of thyroid surgery under local anaesthesia: back to the future? ANZ J. Surg. 72, 287–289 (2002).
5. Malhotra, S. & Sodhi, V. Anaesthesia for thyroid and parathyroid surgery. Contin. Educ. Anaesth. Crit. Care Pain 7, 55–58 (2007).
6. Total Intravenous Anaesthesia – an overview | ScienceDirect Topics. https://www.sciencedirect.com/topics/medicine-and-dentistry/total-intravenous-anaesthesia.
7. Bacuzzi, A. et al. Anaesthesia for thyroid surgery: Perioperative management. Int. J. Surg. 6, S82–S85 (2008).
8. Lentschener, C. et al. Remifentanil-propofol vs. sufentanil-propofol: optimal combinations in clinical anesthesia. Acta Anaesthesiol. Scand. 47, 84–89 (2003).
9. Paquette, C. M., Manos, D. C. & Psooy, B. J. Unilateral Vocal Cord Paralysis: A Review of CT Findings, Mediastinal Causes, and the Course of the Recurrent Laryngeal Nerves. RadioGraphics 32, 721–740 (2012).
10. Rafiq, M., Al-Zoraigi, U., Alzahrani, S. & Alabdulkarim, Y. A Case of Transient Local Anesthetic Induced Bilateral Vocal Cord Palsy. Case Rep. Surg. 2015, 379258 (2015).
11. Tanigawa, K., Inoue, Y. & Iwata, S. Protection of recurrent laryngeal nerve during neck surgery: a new combination of neutracer, laryngeal mask airway, and fiberoptic bronchoscope. Anesthesiology 74, 966–967 (1991).