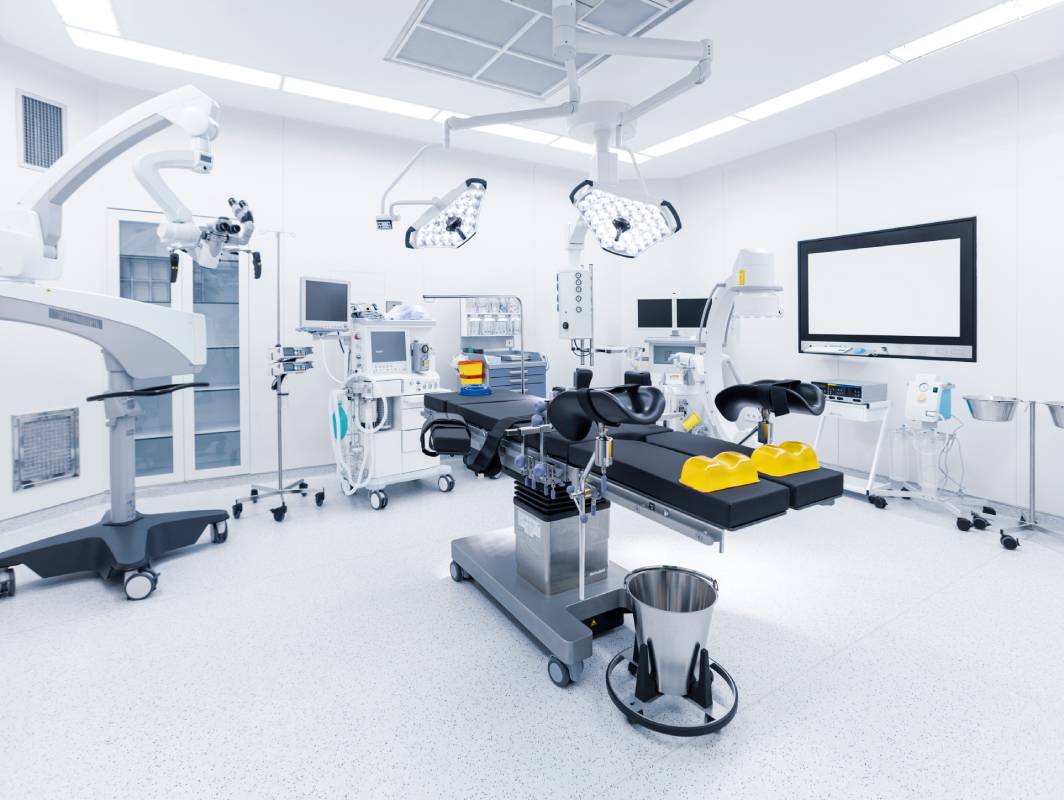
The temperature of an operating room (OR) affects both patient outcomes and the efficiency of surgical procedures. Maintaining an optimal OR temperature is essential for ensuring patient safety, preventing complications, and providing a comfortable environment for the surgical team.
Operating room temperature is crucial for several reasons. First, it affects patient outcomes. Hypothermia is a significant risk during surgery, particularly for patients undergoing lengthy procedures or those with compromised health. Even mild hypothermia can lead to complications such as increased blood loss, infection rates, and extended hospital stays. Maintaining an appropriate OR temperature helps prevent these risks. Second, OR temperature impacts surgical efficiency. A comfortable OR temperature ensures that the perioperative team can perform at their best. Anesthesiologists, surgeons, and supporting providers must remain focused and dexterous, and an overly cold environment can impair fine motor skills and concentration. Finally, OR temperature impacts infection control. Temperature and humidity levels in the OR play a role in controlling the spread of airborne contaminants. Maintaining a balanced temperature helps ensure that the environment remains sterile and reduces the risk of postoperative infections 1,2.
Several factors must be considered when setting and maintaining OR temperatures. Members of the perioperative team may wear multiple layers of sterile clothing, which can make a warmer OR uncomfortable and impair their performance. Additionally, different procedures may have varying requirements for temperature control. The health and age of the patient also influence temperature management, with infants, the elderly, and patients with compromised health requiring more careful temperature regulation to prevent hypothermia.
Typically, the ideal temperature range for an OR falls between 18 and 25°C, with some variation based on the type of surgery and the patient’s condition. The relative humidity, meanwhile, should be about 50%. For surgeries involving significant blood loss or prolonged duration, like cardiovascular and trauma surgery, a slightly higher temperature may be beneficial to help maintain patient body temperature. Since children are more susceptible to hypothermia, OR temperatures for pediatric surgical cases may be set slightly higher 3,4.
Warming blankets or fluid warmers are often used to maintain patient temperature during lengthy or complex surgeries. In addition, modern ORs are equipped with sophisticated HVAC systems that allow precise control of temperature and humidity levels. The use of temperature monitoring devices on patients provides important information to the perioperative team 5.
Maintaining an optimal OR temperature is a delicate balance that requires consideration of patient safety, surgical efficiency, and infection control. By adhering to recommended temperature ranges and adjusting based on the specific needs of the surgery and the patient, healthcare providers can enhance surgical outcomes and ensure a safe, comfortable environment for both patients and providers.
References
1. Hakim, M. et al. The Effect of Operating Room Temperature on the Performance of Clinical and Cognitive Tasks. Pediatr. Qual. Saf. (2018). doi:10.1097/pq9.0000000000000069
2. Why Operating Rooms Are So Cold. Available at: https://www.verywellhealth.com/are-operating-rooms-cold-to-prevent-infection-2549274. (Accessed: 21st May 2024)
3. Operating Theatre Temperature & Humidity Guidelines – Cairn Technology. Available at: https://cairntechnology.com/operating-theatre-temperature-humidity-guidelines/. (Accessed: 21st May 2024)
4. ELLIS, F. P. THE CONTROL OF OPERATING-SUITE TEMPERATURES. Br. J. Ind. Med. (1963). doi:10.1136/oem.20.4.284
5. Broad to Precise Temperature Control for Industry – Air Innovations. Available at: https://airinnovations.com/environmental-control/broad-to-precise-temperature-control-for-industry/. (Accessed: 21st May 2024)