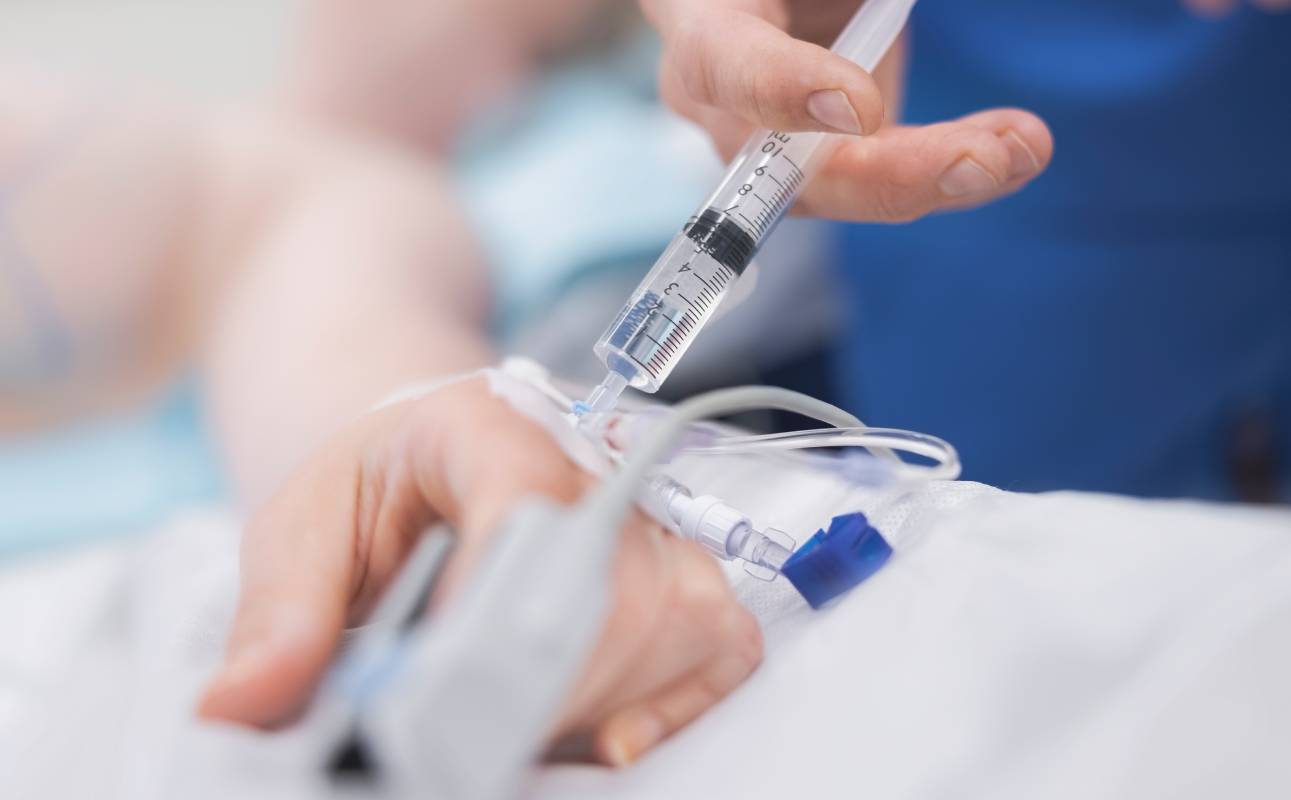
Non-operating room anesthesia, also known as NORA, refers to the use of anesthesia in settings outside of a traditional operating room. Non-operating room anesthesia is used in intensive care, gastroenterology, cardiology, and other areas of medicine for various diagnostic and interventional procedures (2). While NORA offers several benefits, non-operating room anesthesia has been documented to have a higher incidence of malpractice resulting in preventable deaths compared to traditional anesthesia delivered in operating rooms (5). Implementing precautionary measures to ensure patient safety when delivering non-operating room anesthesia can improve patient outcomes as the use of NORA continues to grow.
Despite some of its associated safety concerns, non-operating room anesthesia offers a number of benefits to patients. For example, NORA allows for procedures to be performed in settings that are more convenient and comfortable for patients compared to an operating room, such as a doctor’s office or a clinic. This can reduce the need for hospitalization and result in cost savings for patients. Additionally, NORA can improve patient outcomes by allowing patients to undergo less invasive procedures that can be performed more quickly and efficiently (1).
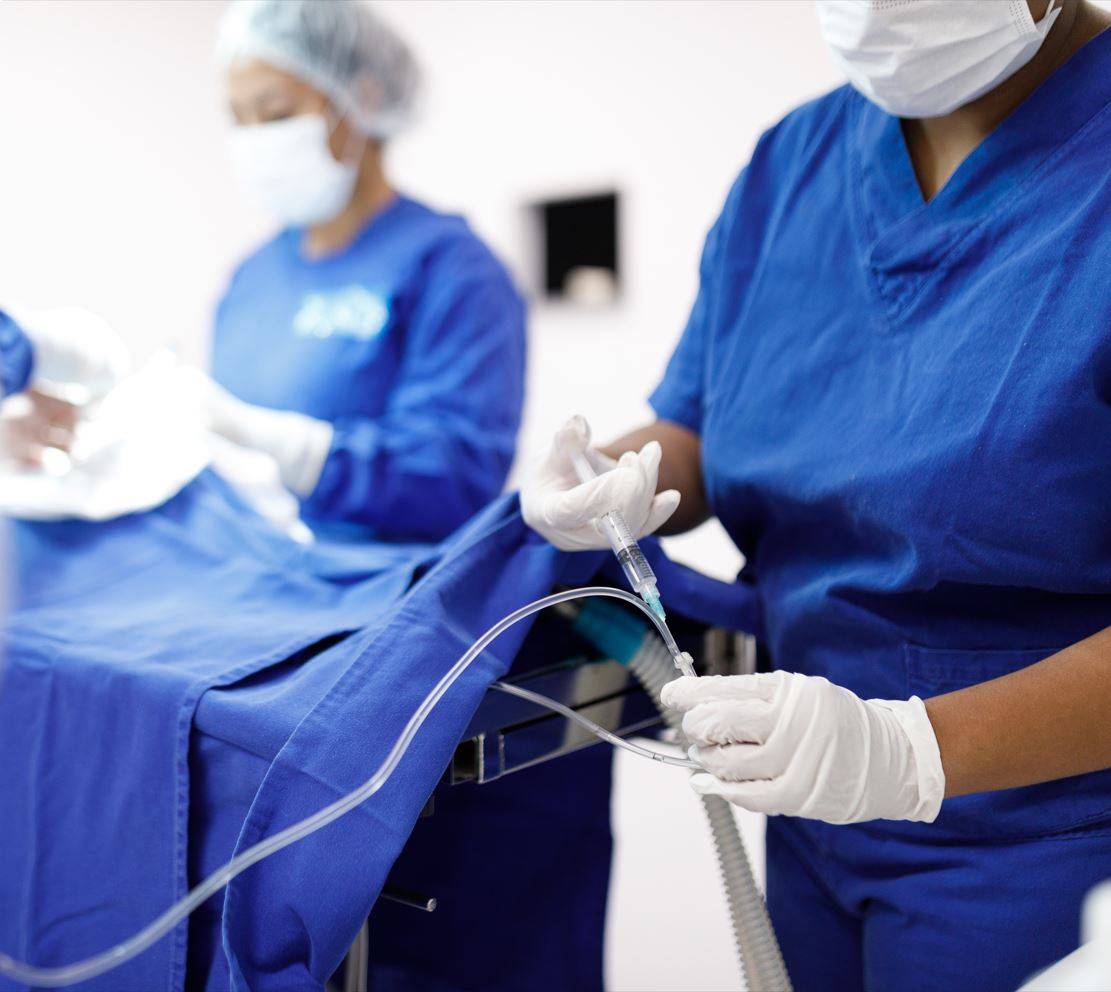
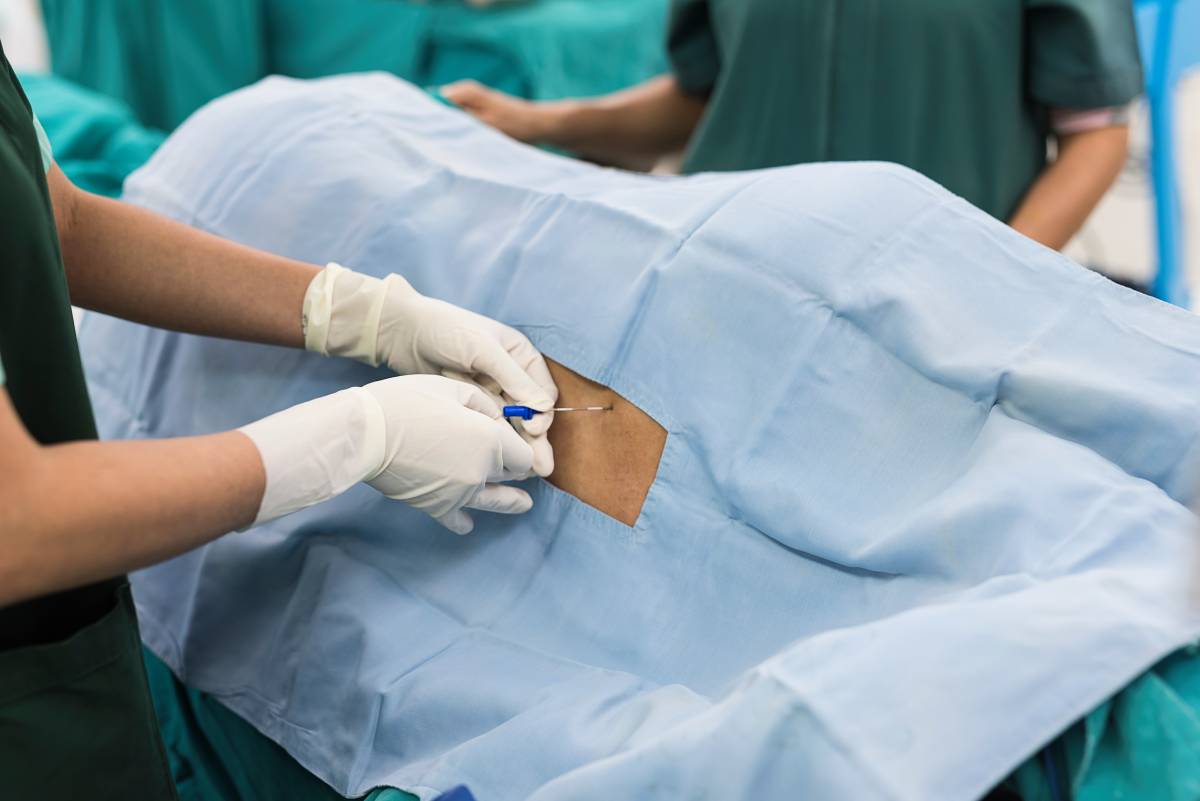
One of the most common issues with non-operating room anesthesia is that procedures performed outside of the operating room may not have the same safety protocols in place as those in a traditional setting (1). The locations where NORA is performed may not have the proper anesthesia equipment necessary to safely deliver anesthesia and monitor patients. Additionally, the location may lack proper lighting or have restricted mobility that limits access to patients (2). There may also be fewer staff with anesthesia training on site compared to a hospital setting (4). A single anesthesiologist may be responsible for providing all aspects of anesthesia care. Malpractice claims for non-operating room anesthesia have a higher rate of death compared to traditional anesthesia (5). Inadequate oxygenation and ventilation are the most common cause of death in NORA settings, accounting for a third of NORA malpractice claims (5). That being said, with proper safety protocols, non-operating room anesthesia is a valuable part of modern medicine.
Improving the safety of non-operating room anesthesia requires diligence on the part of providers and appropriate work environments and safety procedures (2). Providers should take care to assess patient risk prior to administering anesthesia, monitor patients’ vitals during the procedure, and provide proper postoperative care. In particular, intraoperative monitoring needs to be held to the same high standards in place in a traditional operating room to ensure proper oxygenation and circulatory function (4).
Moreover, collaboration between anesthesiologists and staff who are present during non-operating room anesthesia is necessary to develop safety plans when delivering NORA. Conducting comprehensive patient assessments prior to the procedure and offering adequate pain control and postoperative monitoring is essential to improving patient outcomes (4). As technologic advancements in medicine continue to increase, the menu of less invasive procedures suitable for NORA will grow in number. As a result, improved safety measures for non-operating room anesthesia can contribute to higher standards of healthcare for older and high-risk patients (1).
References
- Bonovia et al. “Non-operating room anesthesia in the intensive care unit.” Journal of Clinical Anesthesia, vol. 78, June 2022, doi: 10.1016/j.jclinane.2022.110668
- Herman et al. “Morbidity, mortality, and systems safety in non-operating room anesthesia: a narrative review.” British Journal of Anesthesia, vol. 127, no. 5, pp. 729-744, Nov 2021, doi: 10.1016/j.bja.2021.07.007
- Maddirala, Subrahmanyam, and Annu Theagrajan. “Non-operating room anaesthesia in children.” Indian journal of anaesthesia vol. 63,9 (2019): 754-762. doi:10.4103/ija.IJA_486_19
- Wong, Timothy et al. “Non-Operating Room Anesthesia: Patient Selection and Special Considerations.” Local and regional anesthesia vol. 13 1-9. 8 Jan. 2020, doi:10.2147/LRA.S181458
- Woodward, Zachary G et al. “Safety of Non-Operating Room Anesthesia: A Closed Claims Update.” Anesthesiology clinics vol. 35,4 (2017): 569-581. doi:10.1016/j.anclin.2017.07.003